Click PDF image below to download
Introduction
Permanent facial paralysis is rare, and it occurs due to severe facial nerve branch damage. The facial nerve consists of five primary branches: frontal, zygomatic, buccal, marginal mandibular and platysmal. Long-term facial paralysis is most frequently associated with damage to the frontal nerve branch, but extensive damage to any of the facial nerve branches may lead to permanent facial paralysis.
Permanent facial paralysis has also been linked to tumor removal. For example, a surgeon may alter a patient’s facial nerve to safely remove a cancerous tumor. If a surgeon inadvertently damages the facial nerve, a patient may experience long-term facial paralysis after his or her tumor is removed.
Facelift surgery patients may be susceptible to permanent facial paralysis, too. Research indicates the overall risk of permanent facial nerve paralysis following facelift surgery ranges from 0.53% to 2.6%.
Permanent facial paralysis sometimes occurs, but help is available. At The Facial Paralysis Institute, we offer treatments to address permanent facial paralysis. We also educate our patients about all aspects of permanent facial paralysis and help them find the best way to treat their facial paralysis symptoms.
To better understand permanent facial paralysis, let’s examine the condition, its short- and long-term effects and how it is treated.
What Is Permanent Facial Paralysis?
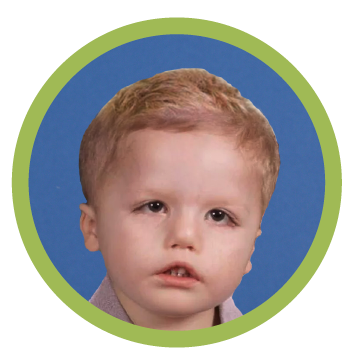
Permanent facial paralysis is a condition that results in the loss of facial movement. It often causes facial muscles to droop or weaken. Also, permanent facial paralysis may affect one or both sides of the face.
The onset of facial paralysis symptoms varies, too. Bell’s palsy patients sometimes start to experience facial paralysis symptoms within 48 hours of onset. Conversely, an individual dealing with a head or neck tumor may gradually experience facial paralysis over the course of several months.
Causes of Permanent Facial Paralysis
There are many reasons why permanent facial paralysis occurs, and these reasons include, but are not limited to:
1. Bell’s Palsy
Approximately 40,000 Americans experience Bell’s palsy annually, according to the National Institute of Neurological Disorders and Stroke. Bell’s palsy symptoms range from mild to severe, and they include facial weakness, twitching and paralysis. Sometimes, Bell’s palsy patients also experience impaired speech, dizziness, ringing in one or both of the ears, headaches and loss of taste. While approximately 85% of Bell’s palsy patients recover completely, there is a chance that the facial paralysis from Bell’s palsy will be permanent.
2. Stroke
A stroke occurs when nerves that control facial muscles are damaged in the brain. This limits the flow of blood and oxygen to the brain, which may lead to facial drooping, numbness and other facial paralysis symptoms.
3. Lyme Disease
Lyme disease is a bacterial infection spread by ticks. Within three to 30 days of a tick bite, bacteria from the bite site will spread within a person’s body. This often results in muscle pain, joint pain and fatigue. It sometimes causes facial paralysis and other neurological symptoms as well.
4. Ramsay Hunt Syndrome
Ramsay Hunt syndrome occurs when a shingles outbreak affects the facial nerve near the ear. When this happens, an individual may suffer a rash, as well as hearing loss and facial paralysis.
5. Acoustic Neuroma
An acoustic neuroma is one of the most common types of brain tumors, and it is located near a nerve between the inner ear and brain stem. An acoustic neuroma is non-cancerous, but facial paralysis sometimes occurs if a large tumor is present or when the tumor is surgically removed. Additionally, an acoustic neuroma compresses the brain stem over time. If an acoustic neuroma goes untreated, it can be fatal.
6. Moebius Syndrome
Moebius Syndrome is a neurological disorder that often affects the sixth and seventh cranial nerves. The condition frequently results in bilateral facial paralysis, but in some instances, unilateral facial paralysis occurs. Moebius Syndrome is congenital, and there is no cure for the condition. However, surgery sometimes improves a Moebius Syndrome patient’s ability to smile and make other facial expressions.
7. Autoimmune Disease
Autoimmune diseases have been linked to permanent facial paralysis. These diseases include multiple sclerosis, which disables nerves in the brain and spinal cord, and Guillain-Barré syndrome, which damages the immune system.
A facial paralysis diagnosis is key for individuals dealing with any of the aforementioned conditions. If an individual understands the different types of facial paralysis symptoms, he or she can act quickly to treat these issues.
Symptoms of Permanent Facial Paralysis
Common symptoms of permanent facial paralysis include:
- Inability to move one or both sides of the face
- Reduced tearing
- Facial drooping and/or weakness
- Slurred speech
- Altered sense of taste
- Drooling
- Pain behind or in the ear
- Difficulty drinking and/or eating
If a person experiences one or more of the aforementioned facial paralysis symptoms, it is important to consult with a doctor. At this point, a doctor can evaluate a patient’s facial paralysis symptoms and diagnose this individual accordingly.
If the facial paralysis is determined to be permanent, consulting with a facial nerve expert like Dr. Babak Azizzadeh is crucial. Dr. Azizzadeh is Harvard-trained and possesses dual certification in head and neck surgery (otolaryngology) and facial plastic and reconstructive surgery. He performs a series of tests to assess a patient, and in doing so, can determine the best way to treat his or her facial paralysis symptoms.
How Is Permanent Facial Paralysis Diagnosed?
Comprehensive testing is required to properly diagnosis permanent facial paralysis. Common tests used to evaluate a patient and his or her facial paralysis symptoms include:
1. Ear, Nose and Throat (ENT) Evaluation
An ENT evaluation is used to identify an inner ear infection or a head or neck tumor or malignancy. It may also be used to evaluate Bell’s palsy patients who experience dizziness.
2. Neurologic Assessment
A neurologic assessment is used to evaluate a patient’s movement, reflexes, cranial nerves and level of consciousness. It may be used to assess a patient’s motor function and identify muscle weakness on one or both sides of the body.
3. Hearing Test
A hearing test is used to examine the inner ear. It helps a doctor determine if a patient is dealing with hearing damage or inner ear problems.
4. Vestibular Test
A vestibular test is used to measure a patient’s nerve balance. It allows a doctor to evaluate the status of a patient’s nerve balance.
5. Tearing Test
A tearing test is used to assess a patient’s tearing function. It helps a doctor determine if a patient is capable of producing sufficient tears to keep his or her eye moist.
6. Computerized Tomography (CT) Scan
A CT scan allows a doctor to see inside of a patient’s body. It ensures a doctor can evaluate a patient’s neck and temporal bone and identify any tumors or trauma.
7. Magnetic Resonance Imaging (MRI) Scan
An MRI scan uses a magnetic field and radio waves to produce images inside the boy. It enables a doctor to assess a patient’s internal auditory canal and brain and identify any tumors.
8. Electrophysiologic Test
An electrophysiologic test is used to assess the electric flow of a patient’s heart. Common electrophysiologic tests include electroneuronography (ENoG) tests to evaluate the facial nerve and electromyography (EMG) tests to assess a patient’s muscles and their associated nerve cells.
Following these tests, Dr. Azizzadeh then provides his patient with a personalized treatment designed to provide long-lasting facial paralysis symptom relief.
How Is Permanent Facial Paralysis Treated?
Common permanent facial paralysis treatments include:
1. Selective Neurolysis
Developed by Dr. Azizzadeh, selective neurolysis is the first permanent treatment for patients dealing with Bell’s palsy, synkinesis and other facial paralysis conditions. This smile reanimation surgery helps a patient create a natural spontaneous smile. Selective neurolysis also improves a patient’s non-verbal communication and quality of life.
Selective neurolysis corrects “mis-wiring” of the facial nerves that otherwise causes facial paralysis. During a selective neurolysis procedure, Dr. Azizzadeh uses an EMG to map out a patient’s facial nerves. He then decreases the activity of facial nerves that hinder a patient’s ability to smile. Dr. Azizzadeh also releases a patient’s platysma muscle that pulls down the corner of his or her mouth.
A selective neurolysis procedure is performed at an outpatient surgery center, and there are minimal risks and downtime associated with the treatment. In some cases, selective neurolysis has helped facial paralysis patients achieve results in as little as one day after surgery.
2. Masseter to Facial Nerve Transfer
A masseteric-facial nerve transfer improves facial nerve reanimation. During the procedure, Dr. Azizzadeh makes an incision near the front of a patient’s ear. He next identifies the facial nerve and masseteric nerve and sews them together. This ensures the masseteric nerve supports a paralyzed facial nerve to restore normal facial function.
A masseter to facial nerve transfer procedure is typically performed at an outpatient surgery center. Meanwhile, the results of a masseteric-facial nerve transfer usually become visible within a few months of treatment.
3. Cross Facial Nerve Grafts
Permanent facial paralysis patients under the age of 55 may qualify for cross facial nerve grafts that promote facial movement. A cross-face nerve graft is implanted into a patient’s face, and the implant becomes active within eight to 12 months following the procedure.
During a cross-facial nerve graft procedure, Dr. Azizzadeh harvests nerve grafts from a patient’s sural nerve in his or her lower leg. Dr. Azizzadeh then attaches these nerve grafts to a patient’s facial nerve. Next, gracilis muscle free flap is harvested from a patient’s inner thigh and connected to his or her cross-facial nerve graft and neck arteries or veins.
Patients require physical therapy after cross-facial nerve graft procedures. Physical therapy teaches facial paralysis patients how to perform muscle movements in the paralyzed side of the face.
4. Gracilis Muscle Transplant
A gracilis muscle transplant may be performed on patients dealing with facial paralysis for two years or longer. It is used to treat inactive facial muscles and restore spontaneous facial movement.
During a gracilis muscle transplant, Dr. Azizzadeh makes an incision in front of a patient’s ear, and this incision wraps behind the ear and is discreetly placed along the hairline. Dr. Azizzadeh then lifts fat and skin from a patient’s cheek. He also identifies blood vessels that can be used to provide circulation to a transplanted gracilis muscle. Dr. Azizzadeh next removes a portion of a patient’s gracilis muscle from his or her thigh. He transfers the gracilis muscle to a patient’s face and stitches the muscle in place.
A gracilis muscle transplant is usually performed at an outpatient surgery center, and the initial recovery period lasts about five to 12 days. Also, a patient should expect to see the full results of a gracilis muscle transplant within about six to 12 months of treatment.
The right treatment for permanent facial paralysis depends on the patient. In certain instances, rehabilitation is required to optimize facial paralysis treatment results, too.
What Does Long-Term Facial Paralysis Rehabilitation Involve?
Long-term facial paralysis often causes severe facial nerve damage. As such, facial paralysis surgery alone is sometimes insufficient. Thanks to physical therapy, a patient can alleviate his or her facial paralysis symptoms following surgery. Plus, this individual can use physical therapy to regain control of his or her facial muscles and improve facial symmetry.
With physical therapy, a neuromuscular therapist teaches a permanent facial paralysis patient a series of exercises that he or she can use after surgery. These exercises are tailored to a patient and help this individual quickly and safely achieve his or her desired results.
Different types of physical therapy techniques are used to treat facial paralysis symptoms. At The Facial Paralysis Institute, neuromuscular retraining (NMR) is highly recommended as part of the treatment plan for permanent facial paralysis patients.
NMR involves exercises that teach the brain to coordinate facial muscle movements. During NMR, a neuromuscular therapist shows permanent facial paralysis patients how to move muscles on different parts of the face, including muscles commonly used to help people smile, frown and make other facial expressions. A neuromuscular therapist also teaches permanent facial paralysis patients how to isolate facial muscles; that way, these patients are able to suppress facial muscles that otherwise cause unwanted facial movements.
NMR often proves to be exceedingly valuable to patients dealing with permanent facial paralysis related to Bell’s palsy or other viral infections. In these cases, the facial nerve usually recovers on its own within about three months after an initial diagnosis. If a patient’s facial nerve does not heal properly, NMR can help this individual improve his or her facial muscle coordination.
NMR may be incorporated into a permanent facial paralysis patient’s treatment plan. Dr. Azizzadeh consults with a permanent facial paralysis patient to learn about this individual and his or her facial paralysis symptoms. He also performs tests and crafts a custom treatment plan for his patient.
Dr. Azizzadeh also requests follow-up appointments in the weeks and months after permanent facial paralysis surgery. He uses these appointments to assess a permanent facial paralysis patient’s recovery and help this individual achieve the best-possible treatment results.
Are Permanent Facial Paralysis Treatments Safe and Effective?
Many permanent facial paralysis procedures are available, but the optimal treatment depends on the patient. Ultimately, the goal of a permanent facial paralysis procedure is to help a patient safely and effectively treat his or her facial paralysis symptoms. To achieve this goal, a patient is evaluated prior to treatment.
In addition to conducting various permanent facial paralysis patient tests, Dr. Azizzadeh reviews an individual’s medical history and other pertinent information during a consultation. Dr. Azizzadeh strives to learn as much as possible about a patient so he can provide this individual with a safe, effective treatment.
Dr. Azizzadeh also devotes significant time and resources to take care of his patients. He collaborates with permanent facial paralysis patients at all stages of treatment, ensuring these individuals receive plenty of support.
Dr. Azizzadeh educates his patients about facial paralysis treatments, too. He ensures a permanent facial paralysis patient knows what to expect before, during and after treatment. This allows a patient to set realistic expectations for his or her facial paralysis treatment.
Is It Too Late for a Facial Paralysis Treatment?
There is no need to let facial paralysis symptoms linger. If an individual has been suffering from facial paralysis symptoms for an extended period of time, treatments are available to address these issues.
If a person experiences facial paralysis symptoms, consult with a doctor. If facial paralysis symptoms do not disappear or escalate after eight months, meeting with a facial nerve expert like Dr. Azizzadeh is ideal.
Dr. Azizzadeh works closely with permanent facial paralysis patients. He understands there is no surefire treatment for all facial paralysis symptoms, at all times. Therefore, Dr. Azizzadeh learns about a patient, then creates a personalized treatment plan for this individual. Dr. Azizzadeh and his patient next put this treatment plan into action. If a permanent facial paralysis patient has concerns or questions at any point during treatment, Dr. Azizzadeh is happy to address them as well.
Conclusion
Facial paralysis often affects a person’s ability to communicate with others, as well as his or her facial appearance. Yet facial paralysis symptoms that persist for months or years are treatable. In fact, if a facial paralysis patient consults with Dr. Azizzadeh, this individual can take the first step to permanently address his or her facial paralysis symptoms.
Dr. Azizzadeh is available to meet with a facial paralysis patient and discuss different treatment options. To find out more, please contact us today at (310) 657-2203 to schedule a consultation with Dr. Azizzadeh.
Request your consultation with Dr. Azizzadeh today
Call us at (310) 657-2203 to schedule an appointment.
Schedule a Consultation